Intravitreal Injections
Procedures and Treatments for Eye Conditions in Venice, FL
An intravitreal injection is an in-office procedure that is performed by a retina specialist. This procedure is used to place medication directly into the inside of the eye, a space known as the vitreous cavity. The vitreous contains a gel-like fluid known as the vitreous humor gel. This treatment allows for the administration of high levels of medication to the retina.
What Are Intravitreal Injections Used For?
Intravitreal injections are used to treat a number of retinal conditions. The most common retinal conditions that are treated with intravitreal injections include diabetic retinopathy, age related macular degeneration (AMD) and retinal vein occlusion (RVO). However, intravitreal injections are also used to treat conditions such as choroidal neovascularization (CNV), cystoid macular edema (CME), endophthalmitis, and uveitis. Additionally, in the event of a retinal detachment, a gas bubble can be injected into the eye to aid in the repair of the retina.
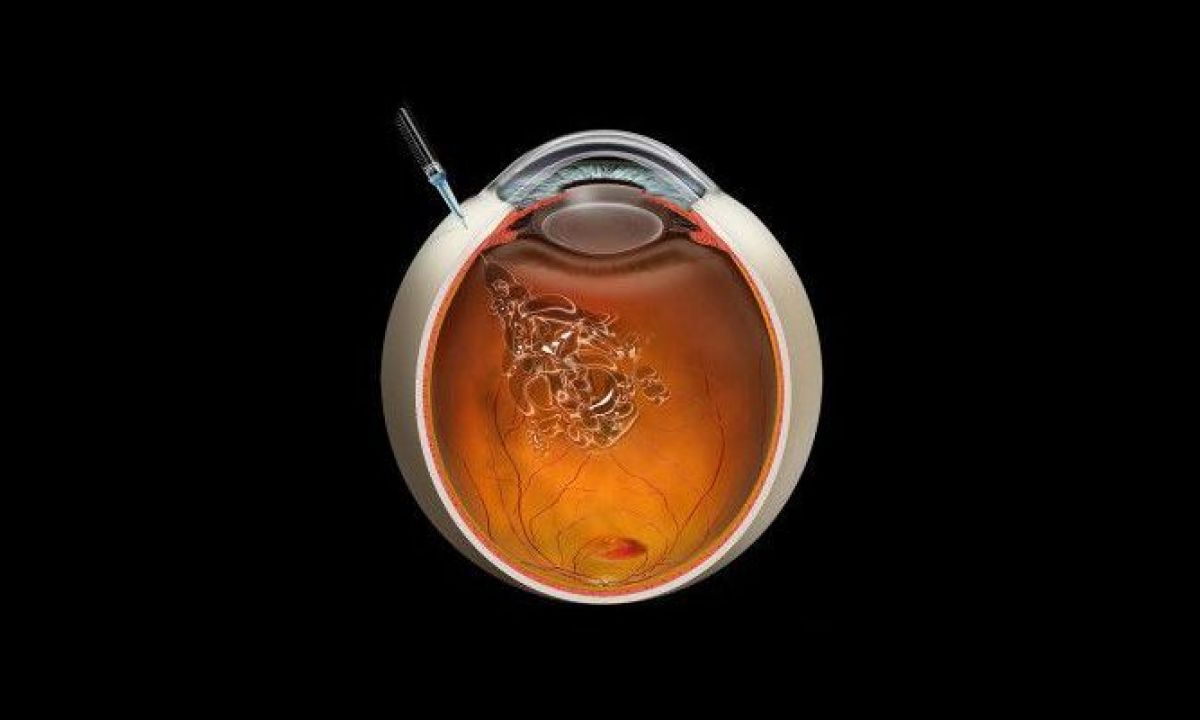
Types of Injections:
Anti-VEGF Drugs:
This group of medication aids in restricting the growth of new blood vessels in the eye. The process of growing new blood vessels is known as neovascularization. VEGF is short for vascular endothelial growth factor. This is a protein that tells the body to grow new blood vessels. However, with conditions such as age-related macular degeneration, the new blood vessels that grow are weak and disrupt places in the eye that can interfere with vision. Anti-VEGF medication inhibits blood vessels from continuing to grow or cause leakage in the eye. Leakage of blood vessels in the eye can lead to loss of vision. The most common anti-VEGF medications administered include Eylea, Avastin, and Lucentis.
Complement Inhibitors:
Newly approved in 2023, complement inhibitors represent a major step forward in the treatment of dry age related macular degeneration. These drugs block part of the immune system responsible for causing damage to photoreceptors, the sensitive retinal cells responsible for vision. Patients who are experiencing advanced dry macular degeneration will preserve their ability to read and drive when treated every 1-2 months with these medications. The first drug of this class to gain FDA-approval is called Syfovre.
Steroids:
Steroid injections are administered to patients who are experiencing active inflammation in the eye that is not sufficiently controlled by the use of steroid drops. These conditions include uveitis, scleritis and cystoid macular edema (CME). Common steroid medications include Triesence, Kenalog and Ozurdex.
Antibiotic, Antifungal and Antiviral Drugs:
This form of injection is administered to patients who have been diagnosed with an infection in the eye. Intravitreal injection of antibiotic medication allows for better access to the site of infection. Injection of antibiotics or antifungal medications is crucial for patients suffering from eye conditions such as endophthalmitis and retinitis. Common medications administered for infections in the eye include vancomycin and ceftazidime.
Intravitreal Gas Injections
Intravitreal gas injections that are completed as an office-based procedure are known as a pneumatic retinopexy. This is a procedure that can be performed on patients with a retinal detachment. The gas bubble covers the site of detachment sealing it off to prevent further damage to the retina.
How Is an Injection Administered?
Intravitreal injections are considered to be an in-office procedure that is performed by a retina specialist. The patient will be reclined back in an exam chair where a drop of betadine will be placed in the eye. This is how the eye is cleaned to reduce the possibility of infections from the bacteria that lives on the surface of the eye. Once the eye has been cleaned, a numbing cotton tip is placed onto the eye at the site of the injection. The numbing medication will help reduce any discomfort that a patient may experience during the injection. A lid speculum is then placed in the eye to keep the eye open during the procedure. The retina specialist will then instruct the patient to look in a specific direction. The injection is then administered into the pars plana of the eye (white portion of the eye) using a small needle.
Usually, the patient will feel pressure in the eye but little to no pain during the injection. After the medication is administered, the speculum will be removed, and the patient will be rinsed with an eye wash solution to remove any residual betadine that may cause discomfort. The entire in office procedure can take anywhere from 2-3 minutes with the injection lasting only a few seconds.
What To Expect After an Injection?
Typically, there are little to no restrictions after an intravitreal injection is given. The patient will be instructed if there are any restrictions after the procedure has taken place. Patients should refrain from exposing the injected eye to potential contaminants the day of the injection. Side effects after an injection are minimal. However, the patient may experience pressure in the eye after the injection or small, temporary floaters immediately after the injection has been administered. Some patients also report surface irritation on the day of their injection.
It is important to contact your retina specialist if you are experiencing one or more of these symptoms after your injection.
- Decrease in vision
- Severe eye pain or discomfort
- Increased floaters after the first day
- Increase sensitivity to light
Patients may also have a foreign body sensation in the injection eye. This may be a side effect to the betadine that is placed in the eye to clean it prior to the injection. Your retina specialist may recommend you use artificial tears for the remainder of the day to ease any surface irritation.
What Are the Risks Of An Eye Injection?
As with any procedure, it is important to know and understand the risk factors associated with intravitreal injections. Although severe complications are uncommon, the major risks to intravitreal injections include:
- Infection in the eye (endophthalmitis)
- Inflammation in the eye (uveitis)
- Vitreous hemorrhage – bleeding into the vitreous gel
- Retinal detachments
Of these adverse events, infection in the eye is the most serious. Symptoms of an infection include worsening pain and vision 1-7 days after an injection. Thankfully, the risk of infection from an eye injection is less than one in 5,000 procedures. In the event of an infection, a patient will receive additional injections of broad-spectrum antibiotics and sometimes surgery to prevent further damage to the eye.
The surface of the eye may also show signs of bleeding at the injection site where the needle enters the eye. This is known as subconjunctival hemorrhage. This side effect will typically go away without intervention within a week. Intraocular pressure may temporarily rise in the eye after an injection is completed. This intraocular pressure will be monitored in the office using a pressure-measurement device until the pressure normalizes.
How Many Injections Will I Need?
Depending on your specific retinal condition, a series of injections may be necessary to better manage your diagnosis. Once a comprehensive eye exam is completed and a retinal condition requiring intravitreal injections has been identified, you and your retina specialist can begin discussing injection intervals. Typically, once an injection has been given for the first time, the patient will be instructed to return to the clinic in 4 – 6 weeks to undergo repeat diagnostic testing. This testing may include ocular coherence tomography (OCT) and/or fluorescein angiography (FA). The use of these diagnostic tools will allow your retinal specialist to better assess how you responded to an intravitreal injection. Using this information, your retina specialist can guide you towards a correct treatment plan.
How Can Venice Retina Help You?
Dr. Anita Shane at Venice Retina is specialized in performing intravitreal injections for a number of retinal conditions. For more information on intravitreal injections or to schedule an appointment, please contact our office.

